By PharmaCompass
2020-10-08
Impressions: 88816
This week, Phispers has more updates on Covid-19 vaccines and therapies.
In the US, President Donald Trump contracted the virus and subsequently returned to the White House after undergoing treatment at a hospital for four days.
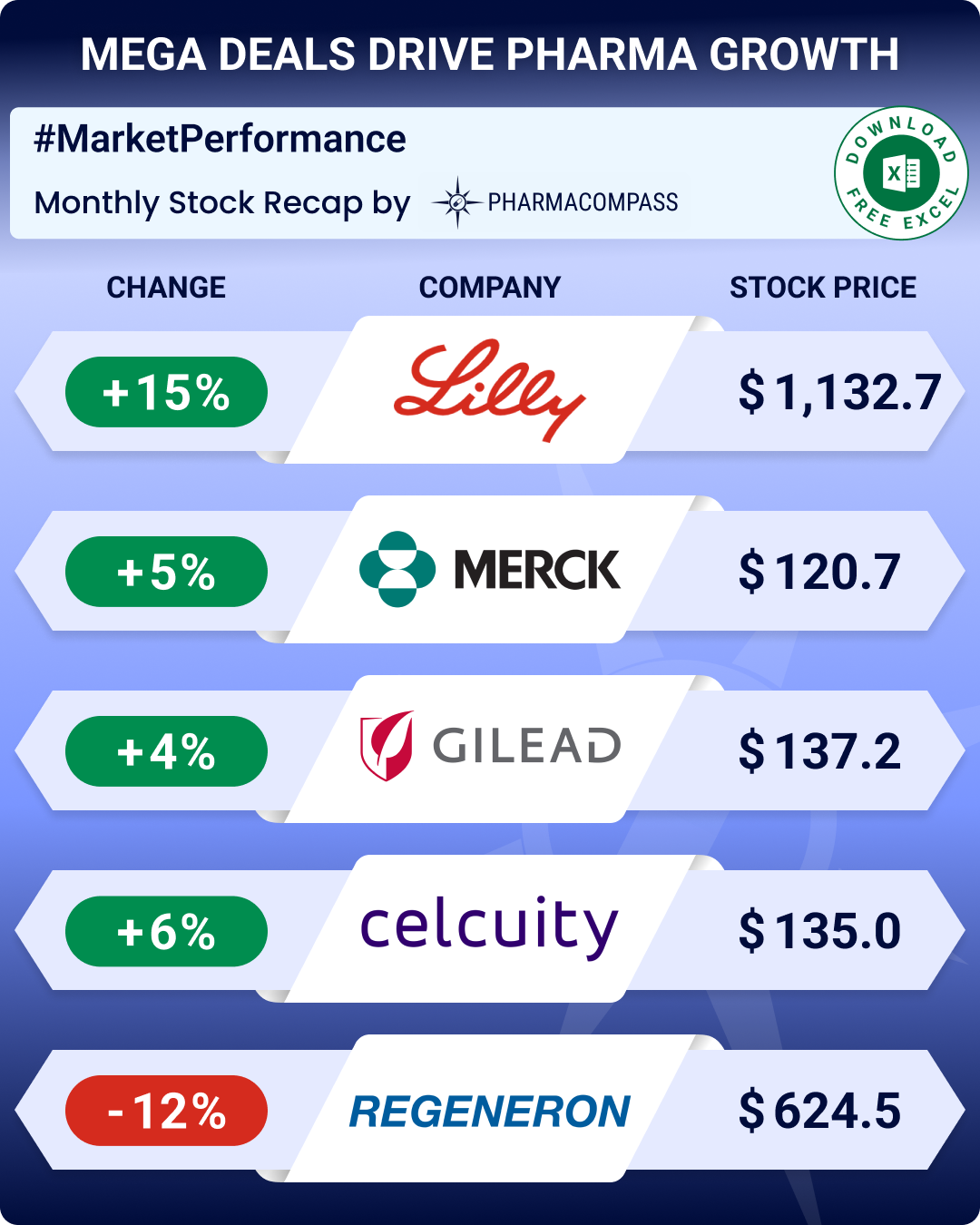
Trump vouched for Regeneron’s experimental monoclonal antibody treatment and has promised to give access to the therapy, free of cost, to all Covid patients in America.
The WHO chief said there is hope that a vaccine against Covid-19 may be ready by the end of the year.
After acquiring Celgene last year, BMS has bought MyoKardia for US$ 13.1 billion in cash.
Three scientists won the Nobel Prize in Physiology or Medicine for identifying the hepatitis C virus, while the Nobel Prize in Chemistry was awarded to two scientists for developing a revolutionary gene-editing tool, the CRISPR/Cas9 genetic scissors.
The USFDA has found high levels of impurity in injectable diuretic acetazolamide.
And while some European countries are facing a shortage of Gilead’s remdesivir, the US is witnessing excess supply of the antiviral drug.
As a result, Gilead will now be selling remdesivir to American hospitals directly.
BMS buys biopharma firm MyoKardia for US$ 13.1 billion
This week, Bristol Myers Squibb and MyoKardia Inc announced a definitive merger agreement under which the former will acquire the latter for US$ 13.1 billion.
The transaction was unanimously approved by the boards of both Bristol Myers Squibb and MyoKardia and is anticipated to close during the fourth quarter of 2020. Bristol Myers will utilize some of the US$ 20 billion in cash and equivalents it had at the end of June for this deal.
MyoKardia is a clinical-stage biopharmaceutical company discovering and developing targeted therapies for the treatment of serious cardiovascular diseases.
With the deal, Bristol Myers gains mavacamten, an experimental heart disease therapy with blockbuster potential. The drug is being tested for treating obstructive hypertrophic cardiomyopathy — a disease where a heart muscle thickens and obstructs blood flow. It affects up to 200,000 people across the US and Europe. Bristol Myers’ willingness to pay a hefty premium to buy MyoKardia reflects a belief that mavacamten can be a significant growth driver in the medium to long term.
Nobel Prizes awarded for Medicine and Chemistry
Three scientists —Harvey J. Alter, Michael Houghton, and Charles M. Rice — have won the Nobel Prize in Physiology or Medicine for their discoveries that led to the identification of the hepatitis C virus, which affects more people than HIV worldwide.
Alter is an emeritus researcher at the National Institutes of Health; Rice is a virologist at Rockefeller University; and Houghton is a British virologist at the University of Alberta in Canada.
The three scientists “made a decisive contribution to the fight against blood-borne hepatitis,” the Nobel Assembly said in a press release.
The 10 million Swedish kronor (or US$ 1,118,000) prize was announced at the Karolinska Institute in Stockholm, Sweden.
The Nobel Assembly said the work of Alter, Houghton, and Rice — during the 1970s and 1980s — “revealed the cause of the remaining cases of chronic hepatitis and made possible blood tests and new medicines that have saved millions of lives.”
Alter began his work in the hepatitis field back in the 1960s and 1970s, around the time when the hepatitis B virus was first discovered. Nearly a decade later, Houghton and his co-workers at the pharmaceutical company, Chiron isolated the genetic sequence of the virus through experiments with chimpanzees.
“For the first time in history, the disease can now be cured, raising hopes of eradicating Hepatitis C virus from the world population,” the Nobel committee said in a statement.
According to numbers from the WHO, there are over 70 million cases of hepatitis C around the world with approximately 400,000 deaths per year.
Nobel Prize in Chemistry: A pair of scientists — Jennifer A. Doudna, a biochemist at the University of California at Berkeley, and Emmanuelle Charpentier, a French microbiologist — won the 2020 Nobel Prize in Chemistry on Wednesday for their work on developing a revolutionary gene-editing tool that can change the DNA of plants and animals with extraordinary precision.
Since Charpentier and Doudna discovered the CRISPR/Cas9 genetic scissors in 2012 their use has exploded. This tool has contributed to many important discoveries in basic research, and plant researchers have been able to develop crops that withstand mold, pests, and drought.
Charpentier and Doudna will equally share the prize money of roughly $1.1 million. Because of the coronavirus pandemic, the usual Nobel Prize ceremonies will be held virtually, with winners receiving their medals and diplomas in their home countries.
After valsartan & metformin, concerns emerge over quality of acetazolamide
Over the last two years, we have seen potential carcinogens, such as N-Nitrosodimethylamine (NDMA) and N-Nitrosodiethylamine (NDEA), being found in various drugs, such as valsartan, ranitidine, and of late, metformin.
With the Covid-19 pandemic raging across the world, experts at the US Food and Drug Administration (FDA) have been concerned about the quality of drugs flowing into the US. And, researchers at the University of Kentucky have filed a petition with the FDA to recall one lot of Mylan and Hikma’s versions of the injectable diuretic — acetazolamide — after finding high impurity levels in tested lots. As a result, UK filed a petition on September 30 with the US Food and Drug Administration (FDA) to recall identified lots of the medication.
After testing acetazolamide in August, researchers found that samples of Mylan's version of the drug contained only 80 to 87 percent of the listed active pharmaceutical ingredient (API). The rest was composed of unknown impurities that UK HealthCare Chief Pharmacist, Philip Almeter called “obscure chemicals that could result from breakdown of product or from reagents used in the manufacturing process.”
In some cases, the impurity levels in Mylan’s version were more than seven times higher than the FDA’s accepted amount. Those findings were later confirmed by AMRI, a contract manufacturer and independent testing lab, the university said.
There is little to no data on the danger these impurities pose as they have not been studied. "Given the unknowns we felt it was important to file the petition with the FDA as soon as possible,” Almeter said. Mylan’s version of the injectable was manufactured in India, while Hikma’s version was made in Portugal.
Meanwhile, drugs are continuously being recalled due to probable cancer-causing impurities. India’s Marksans Pharma has recalled an additional 76 lots of its generic diabetes drug metformin off US shelves after finding high levels of NDMA in more sampled lots. Late last month, Sun Pharmaceuticals recalled one lot of its Riomet ER, an extended-release version of metformin hydrochloride, after finding high NDMA levels.
Drop in demand in US for Gilead’s remdesivir leads to change in distribution
Gilead Sciences is now taking distribution of remdesivir into its own hands. According to a company statement, Gilead will directly sell remdesivir, branded as Veklury, to American hospitals.
Over the last five months, the US Department of Health and Human services was responsible for allocating remdesivir. Starting October 1, drug wholesale company AmerisourceBergen will be the sole distributor of Veklury through the end of the year.
Gilead has been collecting revenue on the drug since July at the wholesale acquisition cost of US$ 3,120 for a typical five-day treatment course. That’s when its US donation of about 1.5 million doses ran out.
At that price, Wolfe Research analyst Tim Anderson projects remdesivir peak sales in both 2020 and 2021 at just below US$ 3 billion. Gilead expects to sell about 1 million to 1.5 million courses this year, which roughly equates to US$ 3.5 billion in revenue.
Gilead quickly worked to ramp up supply by increasing internal manufacturing capacity and by signing on contractors. However, now the supply of remdesivir is exceeding market demand. Gilead is currently seeking full FDA approval for remdesivir in treating Covid-19.
Meanwhile, a Reuters report said European countries, such as the Netherlands, Poland and the UK, are facing shortages of remdesivir because limited supplies are running out. Spain, which has Europe’s highest infection rate, experienced shortages in late August, its medicine agency said. It now has enough doses to meet the needs for the coming weeks, the health ministry said on Tuesday. Britain, which has joined the EU procurement for remdesivir, has rationed its supply, prioritizing Covid-19 patients who need it most, the health ministry said.
Trump avoids HCQ, promises to give Regeneron’s therapy to Covid patients for free
The biggest news that came late last week was that US President Donald Trump had tested positive for the novel coronavirus. What followed this announcement was a mystery behind the medications that were given to Trump by his doctors.
Trump was not given HCQ, convalescent plasma therapy, or even oleandrin, a substance extracted from a toxic shrub and touted as a miracle by Mike Lindell, CEO of MyPillow, a Trump supporter and donor.
Journalist and author Katherine Eban pointed out that instead of hydroxychloroquine (HCQ), oleandrin, or any of the other “shiny objects” his administration has pushed, the president is mixing cutting-edge experimental treatments with a familiar drug that the Pentagon has been studying — famotidine, better known as Pepcid AC.
Trump, who has several risk factors working against him (age, gender, and BMI), was given an 8 gram dose of Regeneron’s monoclonal antibody treatment. Regeneron said it provided the drug to the president in response to a “compassionate use” request from Trump’s doctors.
The founder and CEO of Regeneron, Leonard Schleifer, said Trump’s use of the company’s experimental Covid drug creates “a very tough situation” for the drugmaker since it hasn’t been cleared for broader use.
Before Trump checked out of Walter Reed National Medical Centre to get back to the White House on Monday evening, his doctors had administered the fourth dose of Gilead’s antiviral drug, remdesivir. He had been receiving intravenous infusions of remdesivir since Friday. Typically given to patients with severe infection, it works by hindering the virus’ replication in the body.
Trump was also given dexamethasone, a steroid that the National Institutes of Health’s clinical guidelines recommend for use only in severe cases of Covid-19.
On Wednesday, Trump returned to the Oval Office. He said in a video that he considered getting ill with a virus a “blessing in disguise” because he ended up taking an experimental drug from Regeneron which is still in clinical trials.
Trump suggested that Regeneron’s drug, as well as a similar therapy from Eli Lilly, could soon be authorized for emergency use.
“I want everybody to be given the same treatment as your president, because I feel great,” he said.
He then said everyone should have access to the not-yet-approved drug for “free” and that he would make sure it was in every hospital as soon as possible. “To me it wasn’t therapeutic — it just made me better, OK? I call that a cure,” said Trump.
However, experts point out that there has been no formal publication of Regeneron’s results, not even an unreviewed preprint. All that Regeneron has published are some press releases. Earlier last week, Regeneron had said the treatment improved symptoms and reduced viral loads in non-hospitalized patients who have mild to moderate Covid-19. That was based on results for the first 275 trial patients.
Vaccine Update: WHO says shot may be ready by year-end, EU reviews data in real-time
On Tuesday, the WHO Director-General, Tedros Adhanom Ghebreyesus, said “there is hope” that a vaccine against Covid-19 may be ready by the end of this year. The WHO head called for solidarity and political commitment from all leaders to ensure equitable distribution of the vaccine when it becomes available.
There are nine vaccine candidates in various stages of trials that are part of the WHO-led COVAX global vaccine initiative that plans to distribute 2 billion doses by the end of 2021. A total of 172 countries have joined WHO’s COVAX initiative. However, this excludes the United States, China, and Russia.
EU reviewing real-time data of vaccines: The European Medicines Agency (EMA) is reviewing a Covid-19 vaccine being developed by Pfizer and BioNTech in real time. Last week, the European regulator had launched a similar process for reviewing AstraZeneca’s vaccine.
The EMA is using “rolling reviews” to speed up evaluations of vaccines by studying data as it is submitted, rather than waiting for all data to be made available along with a formal application. Pfizer and BioNTech said the start of the review is based on data from laboratory and animal testing, as well as early testing on humans, while continuing talks to submit data as it emerged.
Uncertainty in US over EUAs before Nov 3: This week, the US Food and Drug Administration (FDA) published briefing documents related to an upcoming advisory committee meeting on Covid-19 vaccines, as well as guidance for the industry.
In these documents, the agency has outlined stricter criteria that need to be met in order to support an emergency-use authorization (EUA) request. According to a New York Times report, White House officials objected to new federal guidelines for the emergency release of a vaccine, including one that would ensure that no vaccine could be authorized before the November 3 presidential election.
However, a few hours later, another report by the same publication said the White House has approved stricter guidelines for vaccine makers. The guidelines make it “highly unlikely that a coronavirus vaccine will be given” an EUA before the election day.
Pfizer’s CEO, Albert Bourla, said in a tweet that “Pfizer has never discussed” FDA’s Covid-19 vaccine guidelines with the White House and will never do so since that could undermine the agency’s independence.
These developments were accompanied by another tweet by an FDA reporter, who said Operation Warp Speed’s scientific head Moncef Slaoui has suggested that AstraZeneca’s vaccine could still win an EUA in late October or early November based on the trials in the UK, Brazil and South Africa. Its trials in the US are still on hold.
Moderna fails to enroll enough minorities in trials: A Reuters report has said Moderna’s vaccine trial contractors have failed to enroll enough minorities (Blacks, Latinos and Native American participants) as volunteers. And this could slow down the approval process. To make up for the shortfall, Moderna slowed enrollment of its late-stage trial and instructed research centers to focus on increasing participation among minority volunteers, the company said.
Covid-19 infects Blacks in the United States at nearly three times the rate of white Americans, and they are twice as likely to die from the virus, according to a report by the National Urban League and other studies. During the last two weeks of September, Moderna said it increased the proportion of Black enrollment, but declined to provide details.
The PharmaCompass Newsletter – Sign Up, Stay Ahead
Feedback, help us to improve. Click here
Image Credit : #Phisper Infographic by SCORR MARKETING & PharmaCompass is licensed under CC BY 2.0
“ The article is based on the information available in public and which the author believes to be true. The author is not disseminating any information, which the author believes or knows, is confidential or in conflict with the privacy of any person. The views expressed or information supplied through this article is mere opinion and observation of the author. The author does not intend to defame, insult or, cause loss or damage to anyone, in any manner, through this article.”