


1. Faricimabum
2. Vabysmo
3. Faricimab-svoa
4. Rg7716
5. Refchem:58354
6. Y8ha1i28d3
7. Qc4f7fkk7i
8. Rg-7716
9. 1607793-29-2
10. Ro6867461
11. Ro-6867461
12. Rg-7716 (antivascular Endothelial Growth Factor/anti-angiopoietin 2 Bispecific Antibody)
13. Gtpl8529
14. Schembl29500934
15. Rg-7713
16. Q27088593
| Molecular Weight | 440.0 g/mol |
|---|---|
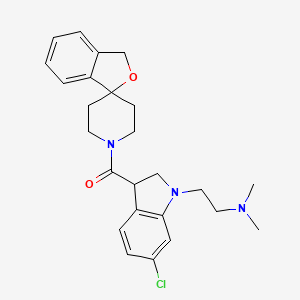
| Molecular Formula | C25H30ClN3O2 |
| XLogP3 | 3.2 |
| Hydrogen Bond Donor Count | 0 |
| Hydrogen Bond Acceptor Count | 4 |
| Rotatable Bond Count | 4 |
| Exact Mass | Da |
| Monoisotopic Mass | Da |
| Topological Polar Surface Area | 36 |
| Heavy Atom Count | 31 |
| Formal Charge | 0 |
| Complexity | 651 |
| Isotope Atom Count | 0 |
| Defined Atom Stereocenter Count | 0 |
| Undefined Atom Stereocenter Count | 1 |
| Defined Bond Stereocenter Count | 0 |
| Undefined Bond Stereocenter Count | 0 |
| Covalently Bonded Unit Count | 1 |
Faricimab is indicated for the treatment of neovascular (wet) age-related macular degeneration (nAMD) and diabetic macular edema (DME).
Vabysmo is indicated for the treatment of adult patients with: neovascular (wet) age-related macular degeneration (nAMD), visual impairment due to diabetic macular oedema (DME), visual impairment due to macular oedema secondary to retinal vein occlusion (branch RVO or central RVO).
Treatment of choroidal neovascularisation secondary to pathologic myopia
Treatment of retinal vein occlusion
Treatment of diabetic retinopathy
Angiogenesis Inhibitors
Agents and endogenous substances that antagonize or inhibit the development of new blood vessels.
ATC: S01L
S - Sensory organs
S01 - Ophthalmologicals
S01L - Ocular vascular disorder agents
S01LA - Antineovascularisation agents
S01LA09 - Faricimab
ATCvet Code
QS - Sensory organs
QS01 - Ophthalmologicals
QS01L - Ocular vascular disorder agents
QS01LA - Antineovascularisation agents
QS01LA09 - Faricimab
Absorption
Faricimab unbound plasma Cmax are estimated to be 0.23 0.07 and 0.22 0.07 g/mL in nAMD and DME patients, respectively; these plasma levels are achieved approximately two days post-dose (Tmax). Following repeated intravitreal administration on a q8w schedule, mean plasma trough free faricimab concentrations are predicted to be 0.002-0.003 g/mL. No accumulation is expected in either the vitreal fluid or plasma.
Route of Elimination
Faricimab elimination has not been fully characterized; faricimab may be excreted renally following its breakdown into smaller peptides and amino acids through cellular catabolism.
Faricimab metabolism has not been fully characterized; as an antibody, faricimab is expected to be catabolized like endogenous immunoglobulins.
Faricimab has an estimated mean apparent systemic half-life of 7.5 days.
The retina is largely avascular to facilitate effective photoreceptor function; rather, the retina is fed by both retinal and choroidal capillary networks, pathologies of which result in retinal and choroidal vascular diseases such as diabetic macular edema (DME), age-related macular degeneration (AMD), and retinal vein occlusion (RVO). One of the underlying causes of retinal vascular diseases (RVDs) is retinal neovascularization (NV), the aberrant growth of new vasculature, usually due to sustained retinal ischemia and mediated primarily by vascular endothelial growth factor A (VEGF-A). VEGF-A is a VEGF family member, which also includes VEGF-B, -C, and -D, whose members signal through the VEGF receptors (VEGFRs) VEGFR-1, -2, and -3 to mediate endothelial and lymphatic growth. Extensive work in animal models of RVD has demonstrated that VEGF-A is necessary but not sufficient in many cases to mediate NV, suggesting that additional factors may be required in deep retinal capillary beds. One such factor has been identified as the angiopoietins Ang-1 and Ang-2 and their cellular receptor Tie-2; Ang-1 is a full Tie-2 agonist whose binding results in Tie-2 phosphorylation and downstream signalling, whereas Ang-2 is a Tie-2 partial agonist/antagonist that inhibits Tie-2 phosphorylation. Ang-1 generally has a protective effect, making endothelial cells less responsive to VEGF-A, while Ang-2 increases VEGF-A-dependent NV and stimulates pericyte apoptosis and breakdown of both the blood-brain and blood-retinal barriers; Ang-2 is upregulated in retinal vascular development and retinal ischemia. Faricimab is a bispecific antibody (bsAb) based on human IgG1 comprising two different heavy and two different light chains capable of simultaneously binding to both VEGF-A and Ang-2 produced using the "CrossMab" platform. Faricimab binds VEGF-A and Ang-2 with binding affinities (KD) of approximately 3 and 22 nM, respectively; importantly, faricimab does not detectably bind Ang-1. Also, the faricimab Fc region has been modified to reduce binding to FcR and FcRn receptors. The former virtually eliminates immune-mediated functions such as antibody- and complement-dependent cytotoxicity and antibody-dependent phagocytosis, whereas the latter increases faricimab systemic clearance by reducing FcRn-mediated IgG recycling. Thus, faricimab works by depleting both VEGF-A and Ang-2 to prevent retinal NV in the privileged ophthalmic environment.
